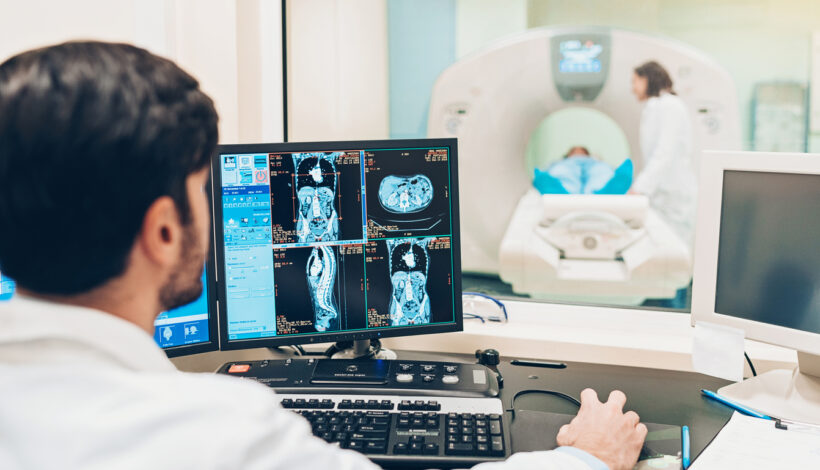
The radiology field is poised for several transformative developments in the coming decade, with advancements in technology, artificial intelligence (AI), and personalized medicine driving significant changes. Here are some potential game changers:
AI and Machine Learning Integration: AI algorithms will continue to revolutionize radiology by enhancing image interpretation, improving accuracy, and expediting diagnosis. These technologies will assist radiologists in detecting abnormalities, prioritizing cases, and providing quantitative analysis, ultimately leading to more efficient and precise patient care.
Quantitative Imaging: There will be a shift towards quantitative imaging techniques that provide more objective and reproducible measurements of disease characteristics, such as tumor volume, perfusion, and metabolic activity. This will enable better treatment planning, response assessment, and prognostication in conditions like cancer, cardiovascular disease, and neurological disorders.
Advancements in Imaging Modalities: Emerging imaging modalities, such as molecular imaging, spectral CT, and functional MRI, will offer deeper insights into biological processes at the cellular and molecular levels. These technologies will facilitate early detection, characterization, and treatment monitoring of various diseases, leading to improved patient outcomes.
Point-of-Care Imaging: Portable and handheld imaging devices will become more prevalent, allowing for rapid and convenient imaging at the bedside or in remote locations. These point-of-care devices will facilitate timely diagnosis and decision-making, particularly in emergency and critical care settings.
Precision Radiology and Personalized Medicine: Radiomics, radiogenomics, and other precision medicine approaches will enable the extraction of valuable quantitative data from medical images, leading to personalized treatment strategies tailored to individual patient characteristics and disease biology.
Enhanced Collaboration and Integration: Radiology will increasingly collaborate with other medical specialties, such as pathology, genomics, and molecular biology, to provide comprehensive diagnostic and therapeutic solutions. Interdisciplinary teams will work together to integrate imaging findings with clinical data, leading to more holistic patient management.
Patient-Centric Care: There will be a greater emphasis on patient-centered imaging, focusing on safety, comfort, and communication. Radiologists will play a more active role in patient education, shared decision-making, and follow-up care, ensuring a positive and empowering experience for patients undergoing imaging examinations.
Overall, the next decade promises to be an exciting and transformative period for the radiology field, with innovations in technology, AI, and personalized medicine driving improvements in diagnosis, treatment, and patient care.